Microneedle Technology and Transdermal Drug Delivery
Medical patches have been around for a long time, but new versions with tiny needles could revolutionize drug delivery.
Microneedle Patches
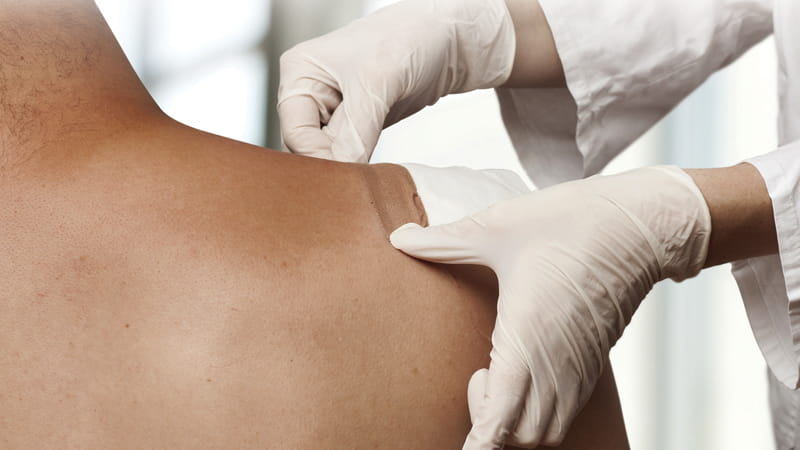
Size: The typical patch is the size of a fingernail or smaller, but it could take any size and shape, depending on the type of drug and dose being administered.
Microneedles: About the width of a human hair with a length of 25 to 2,000 microns. A micron is one-millionth of a meter.
How they work: Can be applied like any bandage. Needles penetrate only the outermost layer of the skin, the stratum corneum.
They can be divided into four types:
- Hollow: These infuse a drug through the bores with adequate flow.
- Solid: These puncture holes in the skin to increase permeability, allowing a drug to then be delivered.
- Coated: These are coated with a drug-containing dispersion.
- Polymer: These are made from special polymers that offer dissolving, non-dissolving or hydrogel-forming options.